Get A Free Legal Consultation
- We fight to maximize your results
- No out-of-pocket costs
- Over $11.7 billion recovered for families



Transvaginal mesh has been used in surgery to treat women suffering from pelvic organ prolapse (POP) and stress urinary incontinence. However, transvaginal placement of surgical mesh, previously believed to rarely cause complications, in fact does result in serious complications, which might require multiple follow-up surgeries to resolve the complications, according to a recent FDA warning.
Women who have experienced serious complications such as mesh erosion, pain, organ perforation and urinary problems may be eligible for compensation through filing a lawsuit.
Pelvic organ prolapse (POP) occurs when the tissues that hold the pelvic organs in place become weak or stretched. Thirty to fifty percent of women may experience POP in their lifetime with two percent developing symptoms. When POP happens, the organs bulge (prolapse) into the vagina and sometimes prolapse past the vaginal opening. More than one pelvic organ can prolapse at the same time. Organs that can be involved in POP include the bladder, the uterus, the rectum, the top of the vagina (vaginal apex) after a hysterectomy and the bowel.
Surgery to repair weakened or damaged tissue is an option for treating pelvic organ prolapse. Some surgeries involve implanting a surgical mesh device into patients in order to reinforce the wall of the vaginal (due to collapse) or to support the urethra (to treat urinary incontinence). Following this procedure, many women have experienced mesh complications.
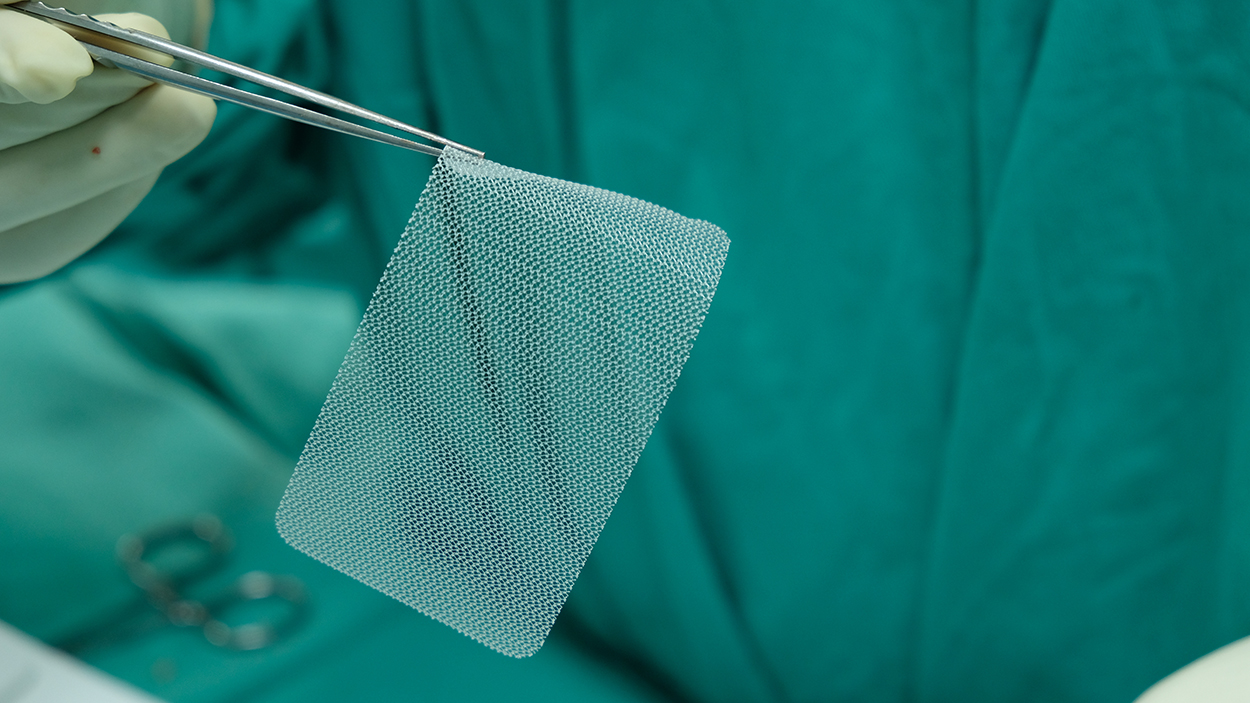
Transvaginal mesh is a type of surgical mesh used to provide support for weakened or damaged tissue inside the body. The mesh is made of either absorbable or non-absorbable synthetic material.
Specifically, transvaginal mesh is used to treat pelvic organ prolapse (POP) and stress urinary incontinence (SUI) in women. When it is used for these conditions, the mesh is surgically implanted to reinforce the vaginal wall (for POP repair) or support the urethra or bladder neck (for SUI repair).
Many women have experienced terrible pain and discomfort related to transvaginal surgical mesh devices. Since October 2008, over 1,000 incidents of transvaginal surgical mesh complications have been reported, according to the Food and Drug Administration.*
A direct connection has been established between transvaginal mesh and serious health complications, including:

Treatment may include surgical and other procedures such as:
Because of the seriousness of the above complications, some patients needed multiple surgeries to remove the mesh that eroded into the vagina. This can result in additional medical bills and longer recovery times.
The U.S. Food and Drug Administration (FDA) has received thousands of reports from women who experienced complications associated with the placement of the surgical mesh. Because of this, the FDA has released warnings concerning the health complications, recommending that patients suffering from POP or SUI who might undergo a surgical procedure for transvaginal mesh take certain precautions.
The FDA recommends that patients suffering from pelvic organ prolapse or stress urinary incontinence who have or might undergo transvaginal placement of surgical mesh should take the following precautions:
In July 2011, the FDA issued a safety communication on the serious complications associated with transvaginal placement of surgical mesh for pelvic organ prolapse. The warning informed the medical community and patients that 1) serious complications associated with surgical mesh for transvaginal non-mesh repair of POP are not rare and 2) it is not clear that transvaginal POP repair with mesh is more effective than traditional non-mesh repair.